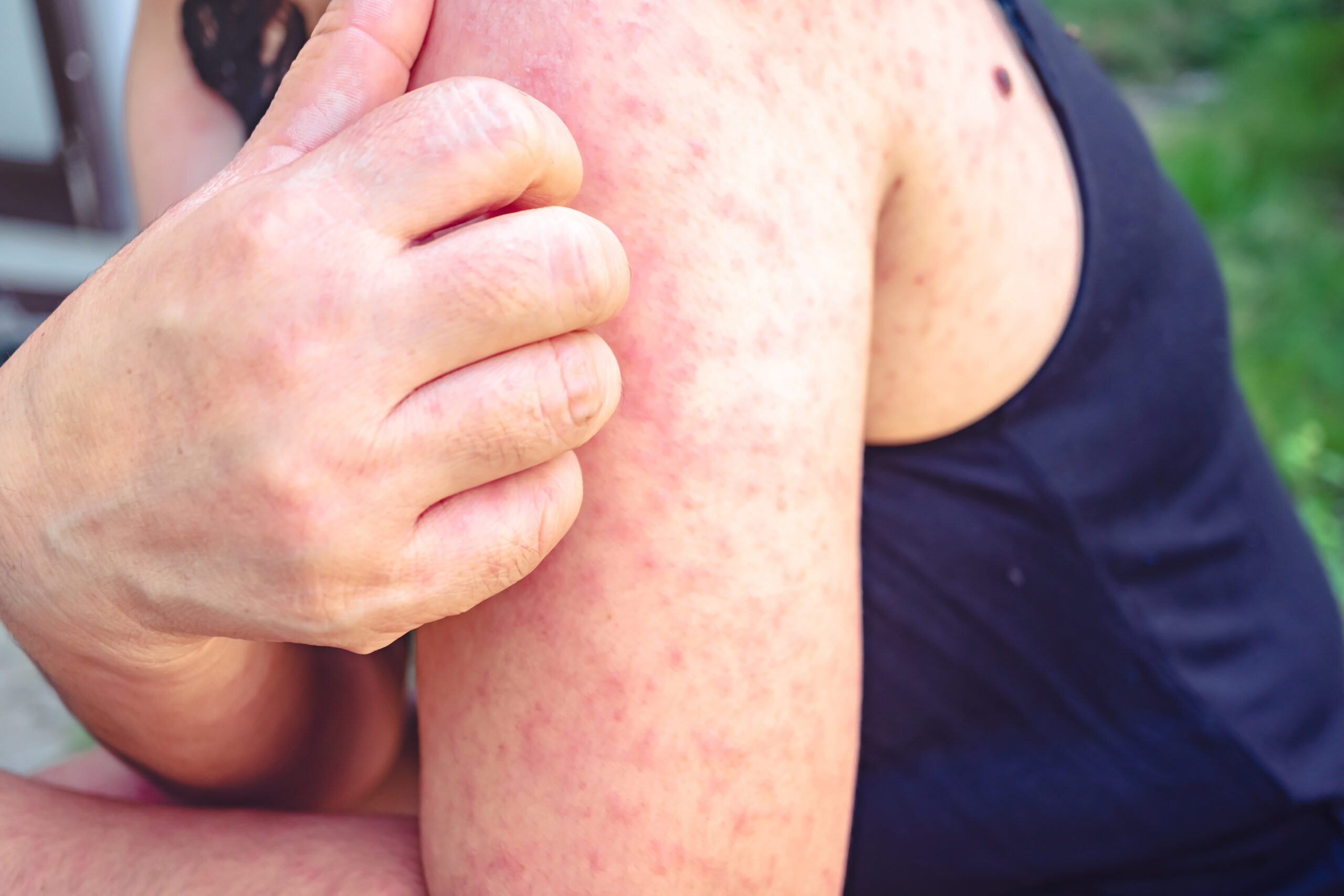
Analysis: antibiotics and vaccination all but wiped out such traditional infectious childhood diseases as measles during the 20th century
By Dr Ida Milne, Lecturer in History
In recent weeks, outbreaks of measles in Europe have caused concern for health authorities and set the alarm bells ringing here too. Ireland saw its first measles death in several years this week. This follows four measles cases reported in 2023, two in 2022, none in 2021 and five in 2020. No deaths were reported in any of those years.
The World Health Organisation has warned that Europe is experiencing an “alarming rise” in measles cases. It has advised increased primary vaccination campaigns, and that countries should also implement robust surveillance systems to identify and close immunity gaps. The HSE is actively developing measles vaccination campaigns, possibly for third level students as well as younger children, and has created a Measles National Incident Management Team (IMT).
Measles is an acute viral disease and has been a notifiable disease in Ireland since 1948. It starts with fever, cough, runny nose and red eyes. Days later, a red rash starts on the head and spreads downwards over the face, neck and body. Measles can cause chest infections, febrile convulsions, ear infections, swelling of the brain and brain damage, deafness and death.
Why has it happened? A combination of pandemic disengagement with childhood measles vaccine schedules, and a longer term trend of failing public knowledge of the real threat measles poses to human life or damage it can cause to the human body are part of the reason the vaccination levels have dropped.
In my research, I have looked at how the huge threat once posed by the traditional infectious diseases of childhood – including measles – were all but wiped out over the course of the 20th century. In the Ireland of the 1910s, at the beginning of my research period, there were over 70,000 deaths in any one year, with thousands dying from tuberculosis, pneumonias and bronchitis. Hundreds were killed each year by whooping cough, measles and diarrhoea. In 1918, for example, 640 deaths here were certified to measles.
This has changed enormously. Just before Covid, total mortality on the island had dropped to less than 30,000 each year, and there were no deaths from the common infectious diseases of childhood that had killed so many Irish children at the beginning of the 20th century.
What caused this change? For one thing, vastly improved housing, with less densely occupied houses than the notorious Dublin tenements where infectious disease could spread like wildfire. Occupants of those tenements were often experiencing syndemic conditions, with more than one epidemic circulating at the same time. Better overall health in better sanitary conditions meant children became less vulnerable to disease.
By the 1950s, sulphonamides and antibiotics had been widely introduced, great reducing the numbers of deaths from tuberculosis, measles and other diseases. But a disease like measles could and still caused long lasting damage for many Irish children. Some of those I interviewed became deaf after experiencing measles, and had to spend the rest of their lives communicating through sign language and other means.
The influence of these drugs has been described by several doctors I interviewed for my research as miraculous. It meant, as Dublin GP Dr James Slein told me for the Royal Academy of Medicine in Ireland’s Living Medical History Project, “we had real weapons’.
Belfast paediatrician Dr Claude Field talked of the absolute confidence medical doctors had in the ability of early antibiotics to treat certain diseases, for example, meningitis, in the 1950s. Meningitis is one of the potential complications of measles. Former Minister for Health, Dr Rory O’Hanlon, said that streptomycin “changed the whole face of tuberculosis” and made a huge difference to sufferers in St Mary’s Hospital in Dublin’s Phoenix Park when he was working there in the 1950s.
While antibiotics helped to reduce the number of deaths from measles, the outbreaks still persisted, until vaccination for measles became more common. The measles vaccine was first introduced in Ireland in 1985, and the combined measles, mumps and rubella (MMR) vaccine was introduced in 1988.
In some ways, measles vaccination has been a victim of its own success. People have forgotten how dangerous the disease is, and some parents thought the vaccine either unnecessary in the modern world, or more dangerous than the disease, which is not the case. That said, some vulnerable children – premature babies like my first daughter for example – may have their vaccine schedule delayed. This makes it all the more important that the people around them are vaccinated.
By the 1990s, Ireland experienced pockets of outbreaks of measles in north Dublin and Belfast, amongst other places. My second daughter caught measles in 1995 at ten months, just before her vaccine became due and it was the first case our GP had ever seen. Luckily, her still delicate older sister had by then received the MMR.
Part of the influence for these 1990s outbreaks was Dr Andrew Wakefield’s false study claiming links between autism and measles vaccination, published in the medical journal The Lancet but quickly refuted. The publicity added to an increase in vaccine hesitancy around the world, and damage to vaccination uptake rates.
This trend, and the Covid blip in childhood immunisation, has influenced the reduction in measles vaccination to below the levels considered necessary to cause ‘herd immunity’, or 95% vaccination rates in the case of measles. The Irish level has not slipped as low as some European countries, but is still below the health authorities’ preferred level, at 90%.
Data on the spread of measles in Europe is available from the European Centre for Disease Prevention and Control. Advice on measles is available from the HSE and there is also a WHO factsheet on measles
This piece was originally published by RTÉ Brainstorm on 8th February 2024